IMPACT PROTOCOL: ACCELERATE YOUR REHAB
A Criterion-based approach for transitioning the postoperative knee safely back to impact activities and competition.
This unique protocol is used for rehabilitation of our knee patients following surgery. This protocol was developed by Nathan Lilley PT, MPT, OCS, CSCS and was released by Biomet Sportmedicine in Digital and DVD format in 2007. Impact consists of graded progressive plyometrics beginning at about 12-14 weeks post-operatively extending to the 6-8 month mark.The purpose of the Impact protocol is to take a research derived criterion-based approach to progressing a patient all the way back to their given sport. This protocol is not for all patients and should only be used for individuals looking to return to competitive athletics.
Background
Traditional rehabilitation following knee surgery has always been an ever-evolving practice.Traditional rehab protocols have often utilized a time based approach to treatment progression. This “cookbook” approach has often caused clinicians to push their patients more aggressively than appropriate. Although post-operative time often has a strong influence in progression, not all patients fall within the “norms” at a given point in time. Co-morbidities, age, complications with surgery and even differences between doctors surgical techniques and philosophies all come into play with rehab progression. It is the responsibility of the clinician to constantly assess and reassess the objective status of the patient to ensure patients progress with their rehabilitation appropriately.
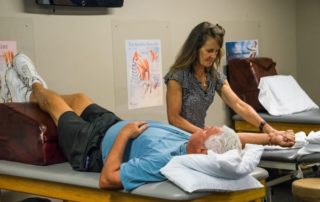
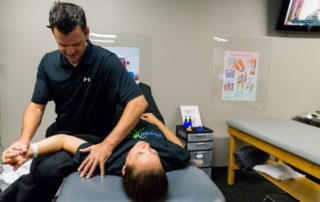
During all phases of the protocol, we are constantly instructing our patients how to minimize faulty movement patterns.
One of the most controversial and challenging dilemma to the clinician is knowing when to safely progress a patient from standard rehab (ROM ,PRE, Proprioception training, Etc.) into impact and more sport specific training. The purpose of the following protocol is to take a research derived criterion-based approach to progressing a patient all the way back to their given sport. Soft tissue healing, graft selection and incorporation, dynamic stability, range of motion, and patient confidence all have be taken into account. Specific clinical “mile stones” have been outlined and must be met before progressing into the next phase of training. Following such guidelines allows us to safely monitor and control the many variables that go into progressing rehab as safely and quickly as possible. The patient should be carefully monitored throughout this progression with the clinician watching for any signs of abnormal joint stress, effusion or pain.
This program consists of graded progressive plyometrics beginning at about 12-14 weeks post-operatively extending to the 6-8 month mark. Once an athlete has completed the protocol they are put through a comprehensive return to sport test. This too is criterion based. If the clinician, athlete and surgeon all agree that the clinical goals are met, then medical release can be considered.
The risk factors of knee injuries have been well documented over the last twenty years.Intrinsic factors such as notch width, tibial slope, recurvatum, and hormonal influences and many other variables are thought to contribute to knee injuries. These are variables that we cannot control as therapists. As clinicians, we turn our focus to the extrinsic variables that can be modified and adapted through training that have been shown to contribute to catastrophic knee injuries. It is the purpose of this protocol to identify and teach our patients such risk factors and how to modify activities to decrease these risks after knee surgery.
It has been estimated that up to 90% of all ACL and knee injuries occur from non-contact mechanisms. Clinical studies have indicated that such injuries usually occur during a landing from a jump or from deceleration prior to a change in direction. Usually this involves an awkward movement or a need to unexpectedly change direction directly prior to the injury. The same studies have shown there usually is an apparent valgus or dynamic valgus in the coronal plane prior to injury. This vulnerable position or “the point of no return” for knee injury has been defined as internal femoral rotation, knee valgus, external tibial rotation, with foot pronation. Knee flexion angles of 45 degrees or less have shown an increase in anterior tibial shear as the quadriceps is contracting eccentrically to slow the landing momentum. Athletes that demonstrate these mechanics are termed ligament dominant and very susceptible to injury.
During all phases of the protocol, we are constantly instructing our patients to minimize these faulty movement patterns stressing that our athletes land with strong athletic positioning utilizing the quads, hamstrings and gluteals to absorb and control the amount of shear at the knee through co-contraction. This form of training is referred to as plyometric exercise.
The Impact Protocol
The first seven weeks of rehab are not outlined. At Physio Pro we use our standard knee protocols for the first seven weeks until the criteria to enter the impact protocol has been met. Patients must meet the entry-level FTA criteria at a minimum of twelve weeks. We will not begin the program sooner 12 weeks post-op. Progression of the program is at the discretion of the therapist/physician. Sound clinical judgment is essential for safe progression. If the criteria are not met then standard therapy will continue until objective measures are adequate.
There are a total of five phases of rehabilitation to complete before a safe return to competition can be considered. Although estimated time frames are outlined, not all patients will progress equally as there may be complicating factors that may hinder or expedite rehabilitation.
Patients must commit themselves to a vigorous but safe 6 to 8 month rehab regime to insure safety and protection of their knee before returning to unrestricted activities.