INSTRUMENTED ASSISTED SOFT TISSUE MOBILIZATION (IASTM)
What is Instrumented Assisted Soft Tissue Mobilization?
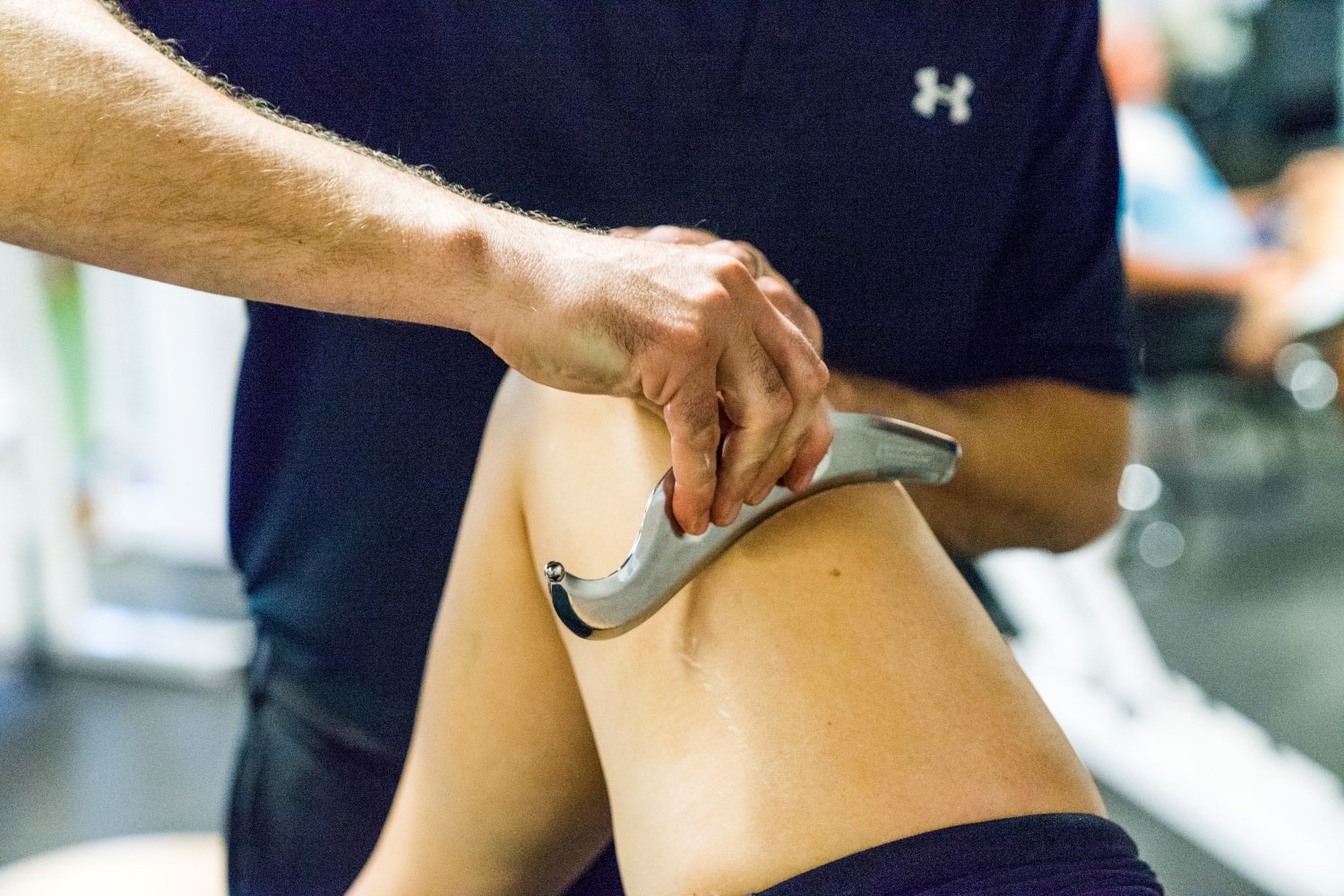
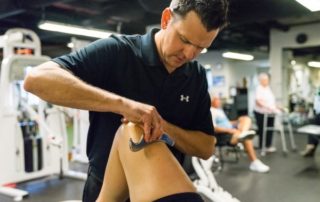
Instrument Assisted Soft Tissue Mobilization (IASTM) is a soft tissue treatment which utilizes various tools that enable the clinician to efficiently locate and treat individuals diagnosed with soft tissue dysfunction. IASTM is performed with specifically designed instruments that are designed to detect and treat fascial restrictions or increased muscular tone. IASTM is a great adjunct to traditional physical therapy interventions prescribed to correct biomechanical deficiencies.[10]
How does it work?
IASTM tools have been shown to effectively break down fascial restrictions and scar tissue. The ergonomic design of these instruments provides the clinician with the ability to locate restrictions and allows the clinician to treat the affected area with the appropriate amount of pressure and to treat the specific direction of restriction. Studies have also showed clinical benefits of IASTM showing improvements in range of motion, strength and pain perception following treatment. Melham et al. found that IASTM significantly improved range of motion in a college football player following 7 weeks of IASTM and physical therapy.[8] Melham et al. found that scar tissue surrounding the lateral malleolus was reduced and remodeled structurally following IASTM application. Wilson et al found improvement in pain reduction and impairment scale at 6 & 12 weeks following IASTM application for patellar tendonitis.[9]
The introduction of controlled microtrauma to affected soft tissue structure causes the stimulation of a local inflammatory response. Microtrauma initiates reabsorption of inappropriate fibrosis or excessive scar tissue and facilitates a cascade of healing activities resulting in remodeling of affected soft tissue structures. Adhesions within the soft tissue which may have developed as a result of surgery, immobilization, repeated strain or other mechanisms, are broken down allowing full functional restoration to occur.[10]
Indications:
- Limited motion
- Pain during motion
- Motor control issues
- Muscle recruitment issues
References
- Fowler, S, Wilson, J, and Sevier, TL, Innovative approach for the treatment of cumulative trauma disorders, Work. 2000; 15:9-14
- Sevier, TL, Helfst, RH, Stover, SA, and Wilson, JK. Clinical trends on tendinitis. Work. 2000; 14:123-226
- Sevier, TL, Gehlsen, JK, Wilson, JK, Stover SA, and Helfst RH. Traditional physical therapy versus augmented soft tissue mobilization (ASTM) in the treatment of lateral epicondylitis. Med Sci Sports Exerc. 1995; 27:S52
- Gehlsen, GM, Ganion, LR, and Helfst, RH, Fibroblast responses to variation in soft tissue mobilization pressure, Med Sci Sports ExercfckLR. 1999; 31:531-535.
- Davidson, CL, Ganion, LR, Gehlsen, GM, Verhoestra, B, Roepke, JE, and Sevier TL, Rat tendon morphologic and functional changes resulting from soft tissue mobilization. Med Sci Sports Exerc. 1997; 29:313-319.
- Davidson, CL, Ganion, LR, Gehlsen, GM, Verhoestra, B, Roepke, JE, and Sevier, Rat tendon morphologic and functional changes resulting from soft tissue mobilization. Med Sci Sports Exerc. 1997; 29:313-319.
- Melham, TJ, Sevier, TL, Malnofski, MJ, Wilson, JK, and Helfst, RH, Chronic ankle pain and fibrosis successfully treated with a new non-invasive augmented soft tissue mobilization (ASTM): A case report. Med Sci Sports Exerc. 1997; 30:801-804
- Wilson, J., Sevier, T., Helfst, R., Honing, E., & Thomann, A. (2000). Comparison of rehabilitation methods in the treatment of patellar tendinitis. J Sports Rehabil, 9(4), 304-314.
- Snodgrass S.J. Thumb pain in physiotherapists: potential risk factors and proposed prevention strategies. J of Manual and Manipulative Therapy 2002;10(4):206-217.
- http://www.physio-pedia.com/Instrument_Assisted_Soft_Tissue_Mobilization#cite_ref-2